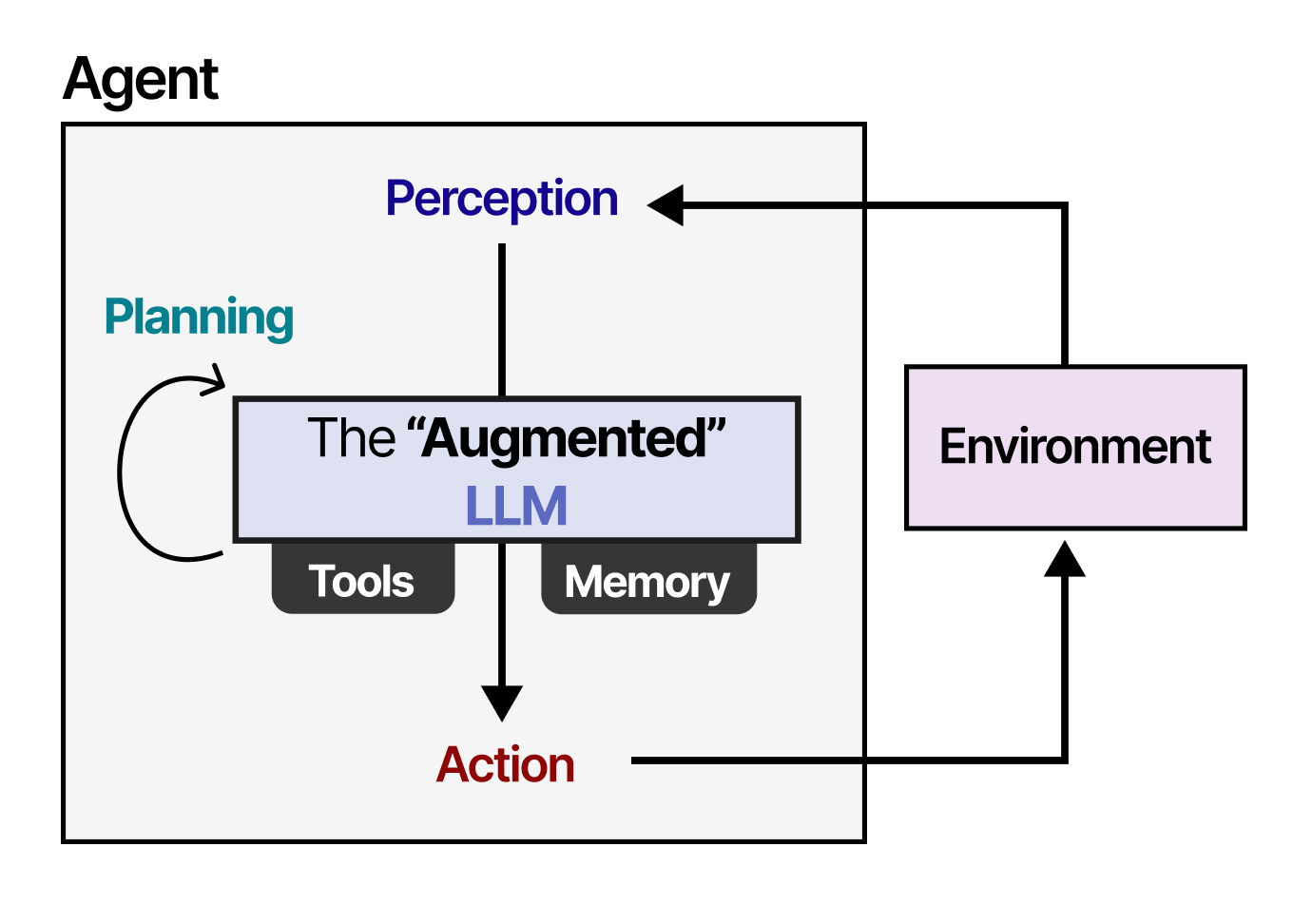
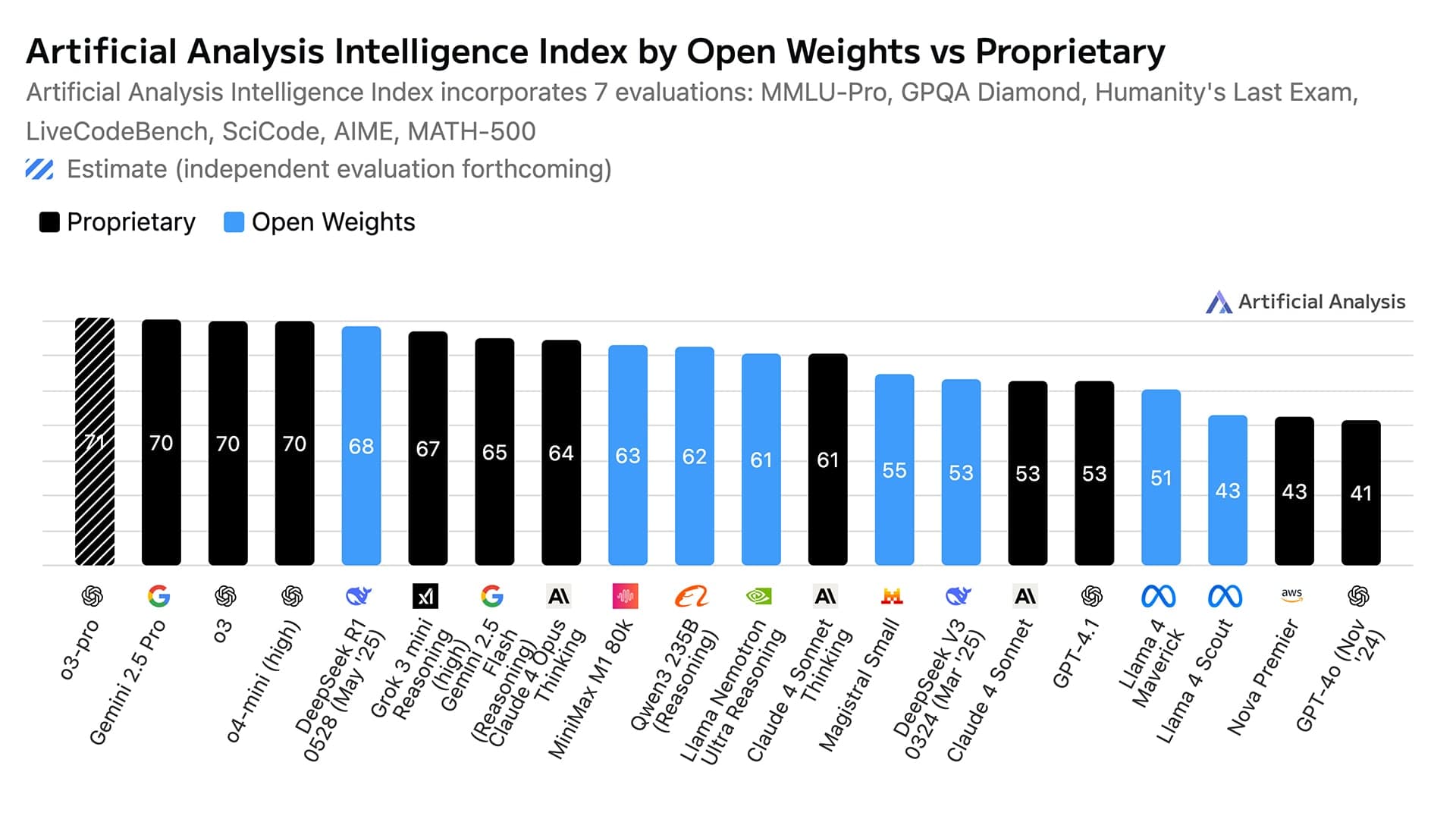
A BBC investigation has highlighted a significant shift in how people seek health information: AI chatbots are becoming a "real front door" for initial health advice. The report, amplified by AI researcher Rohan Paul, notes this trend is accelerating as general-purpose and specialized health AIs become more accessible. However, the investigation also surfaces new evidence suggesting that purely AI-driven interactions may have limitations, and that systems combining human oversight with AI assistance—human-AI hybrids—are showing promise for delivering better, safer outcomes.
Key Takeaways
- The BBC reports AI chatbots have become a major front door for health advice.
- New evidence indicates hybrid human-AI systems outperform pure AI models in healthcare contexts.
What the BBC Found
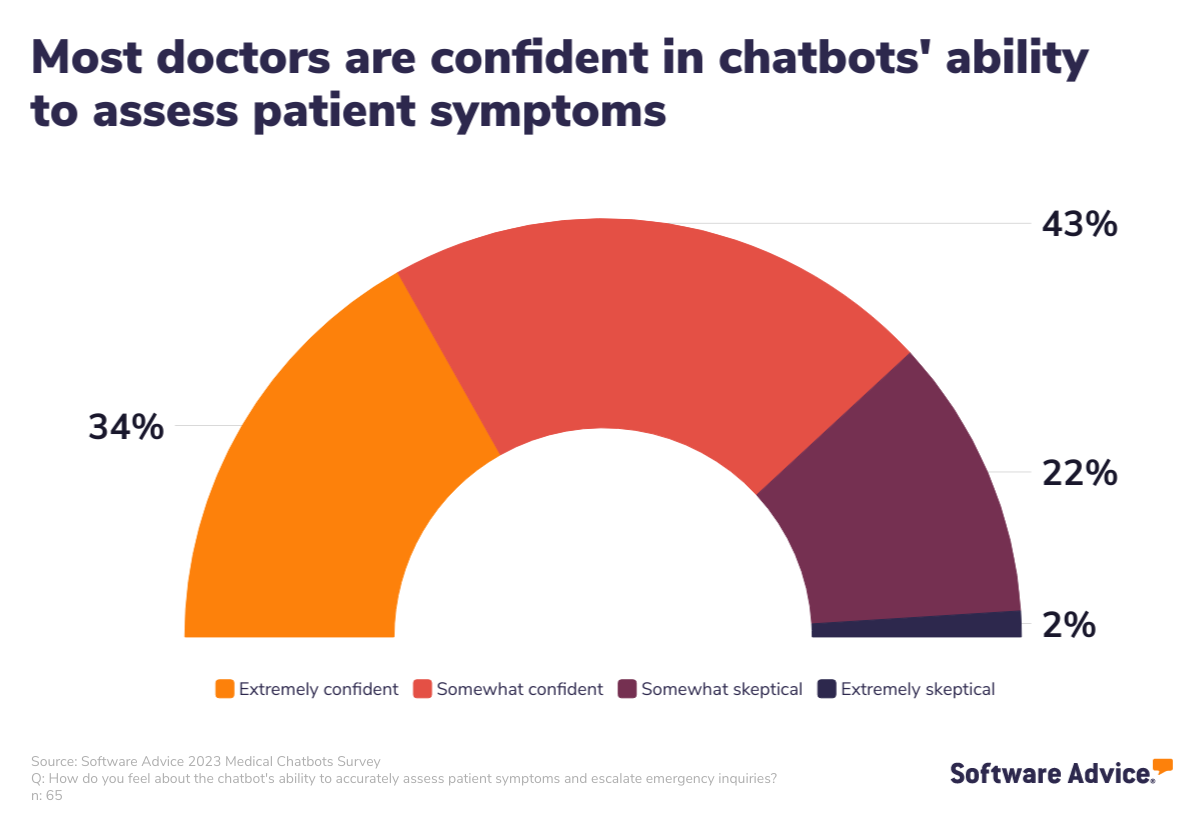
The core finding is behavioral: for a growing number of people, the first step after experiencing a symptom is no longer a Google search or a call to a doctor's office, but a conversation with an AI chatbot. This includes platforms like ChatGPT, Claude, and specialized health-focused AIs from companies like Babylon Health, Ada Health, and others. The convenience, 24/7 availability, and non-judgmental nature of these interfaces are driving adoption.
The investigation points to the dual nature of this trend. On one hand, it can improve access to basic health information and triage. On the other, it raises critical questions about accuracy, liability, and the potential for AI to miss nuanced symptoms or provide harmful advice.
The Evidence for Human-AI Hybrids
Citing emerging research and pilot programs, the BBC report indicates that the most effective models in digital health are not purely automated. Instead, they are "human-AI" hybrids. In these systems:
- AI performs initial triage and information gathering, asking standardized questions and parsing user descriptions.
- A human healthcare professional reviews the AI's assessment, adds contextual judgment, and provides the final advice or recommendation.
Early evidence from studies and deployments suggests this hybrid approach reduces errors, increases user trust, and leads to more appropriate care pathways than either fully AI-driven or traditional, human-only models operating at scale.
The Practical and Ethical Landscape

This shift creates immediate practical challenges:
- Regulation: Most health AIs operate as "wellness" or "informational" tools, skirting strict medical device regulations. Their rise as a primary entry point pressures regulators to reconsider these boundaries.
- Data Privacy: Health conversations are highly sensitive. The data practices of AI companies hosting these chats are under scrutiny.
- Integration: For the hybrid model to work, seamless digital handoffs between AI and human clinicians are necessary, requiring new workflows and software infrastructure.
The report implies that the industry is at an inflection point. The technology for AI-led triage is here and being adopted. The next phase will be defined by how effectively it can be integrated into responsible, clinically supervised care pathways.
gentic.news Analysis
This BBC report validates a trend we've been tracking since the launch of general-purpose reasoning models like GPT-4. In November 2024, we covered Google's AMIE (Articulate Medical Intelligence Explorer), an AI system trained to conduct diagnostic dialogues. While AMIE showed impressive diagnostic accuracy in simulations, Google researchers consistently emphasized it was a research tool, not a replacement for clinicians—a caveat that aligns perfectly with the BBC's findings on the need for human oversight.
The move towards hybrid models echoes a broader pattern in enterprise AI. In sectors like finance and legal tech, the most successful deployments often use AI for draft generation and initial analysis, with a human expert in the loop for final review and decision-making. Health tech, with its high stakes and complex ethics, was always likely to follow this path.
Critically, this trend creates a new competitive axis. It's no longer just about which AI has the best medical knowledge benchmark score. The winners will be the platforms that best orchestrate the human-AI collaboration—managing handoffs, maintaining context, and ensuring a cohesive user experience from chatbot to clinician. Companies like Teladoc and Amwell, which already combine telehealth with AI tools, are positioned for this shift, while pure-play AI health startups may need to build or partner for clinical integration. The evidence cited by the BBC suggests that without this hybrid layer, adoption of AI health advisors may hit a trust ceiling.
Frequently Asked Questions
What are examples of human-AI hybrid health systems?
Examples include modern telehealth platforms where a patient first interacts with a symptom-checker AI. The AI's analysis and the patient's history are then presented to a doctor or nurse practitioner for a video consultation. The clinician can use the AI's work as a starting point, ask follow-up questions, and make a final assessment. This is different from a fully automated chatbot that provides a diagnosis or care plan without any human review.
Are AI health chatbots regulated like medical devices?
Currently, most are not. In the US, the FDA regulates software that is intended to treat, diagnose, cure, mitigate, or prevent disease as a medical device. Many AI health chatbots are marketed for "informational purposes only" or for general wellness, which places them outside the FDA's strictest regulations. The BBC's report that they are becoming a primary care entry point will likely increase regulatory scrutiny and pressure to clarify these boundaries.
What are the biggest risks of using an AI chatbot for health advice?
The primary risks are accuracy and bias. An AI may hallucinate information, miss subtle cues in a user's description, or lack knowledge of very recent medical research. It may also reflect biases present in its training data. Furthermore, an AI cannot perform a physical examination or interpret non-verbal cues. There is also a risk of over-reliance, where a user accepts potentially incorrect AI advice instead of seeking necessary professional care, or mis-triage, where the AI underestimates the severity of a symptom.
How can I use AI for health information safely?
Treat AI as a preliminary information-gathering tool, not a definitive source. Use it to help formulate questions for a healthcare professional, not to self-diagnose. Always verify any information or recommendations with a credible source like a government health agency (CDC, NHS) or, ultimately, a qualified doctor. Be extremely cautious of any AI that recommends specific medications or treatments without human oversight.